Psychosis is highly stigmatized in our society. People who have psychosis are often considered mad and ostracized. But almost anyone can be affected by psychosis, from the young to the elderly. It’s estimated NIMH that 3% of the population will have some kind of psychosis in their lifetime.
Table of Contents
- What is Psychosis?
- Glossary of Terms
- Digital Recreation and Its Influence on Psychosis
- Types of Psychosis
- Diagnosis of Psychosis Symptoms and Signals
- What Causes Psychosis?
- Diagnostics Used to Assess Psychotic Patients
- Psychosis Treatment
- Useful Resources and International Association
- Questions and Answers
- List of References
Reviewers:

Virginia Chow is a practicing Canadian psychologist. Her main goal is helping people to fight such mental problems as addictions, depression, anxiety and many others. Virginia is a member of the Order of Psychologists of Quebec. The doctor graduated from Concordia University and worked for such medical institutions as St. Mary’s Hospital, Mentis Health Centre and Pavillon Foster. You can also search for this author in Google Scholar or PubMed.

Leonard George is a Canadian researcher and psychologist. His topic of interest is a wide variety of mental health issues and cognitive science. Having received a Ph.D. at the University of Western Ontario, Leonard wrote two works about religious history
and paranormal experience and many articles. Nowadays, he is working at Capilano University, Vancouver. You can also search for this author in Google Scholar or ResearchGate.
What is Psychosis?
Psychosis can occur due to several underlying health conditions. A person experiencing psychosis believes in or hears or sees things that are not real. The person is incapable of distinguishing their reality from their psychoses.
Glossary of Terms
1. Psychosis Definitions
Psychosis is a generalized term covering a wide range of illnesses. And there are several terms associated with psychosis that help to describe symptoms and diseases. Below are some popularly used terms.
2. Psychosis Episode
A psychosis episode is a period when a sufferer experiences hallucinations and delusions. During an episode, a person may be extremely agitated and frightened. They may behave unsafely and be a danger to themselves or others.
3. Negative Symptoms
It means the absence or loss of actions or feelings, such as being demotivated.
4. Positive Symptoms
These include outward symptoms, including hallucinations and delusions.
Schizophrenia
Schizophrenia is a mental disorder that involves a breakdown of reality. Sufferers experience hallucinations and delusions. It is a severe condition that can lead people to commit suicide or behaving aggressively and dangerously. Most patients require continual drug treatment to prevent relapses of delusional thoughts.
5. Hallucinations

A hallucination is a sensory perception that someone experienced in the absence of external stimuli. Hallucinations can be auditory, which means hearing something that isn’t there. Or visual, when a person sees something that isn’t there.
A hallucination is a sensory perception that someone experienced in the absence of external stimuli. Hallucinations can be auditory, which means hearing something that isn’t there. Or visual, when a person sees something that isn’t there.
6. Prodrome
A prodrome is the earliest symptoms that occur in an illness. It is the sign of an onset of a disease.
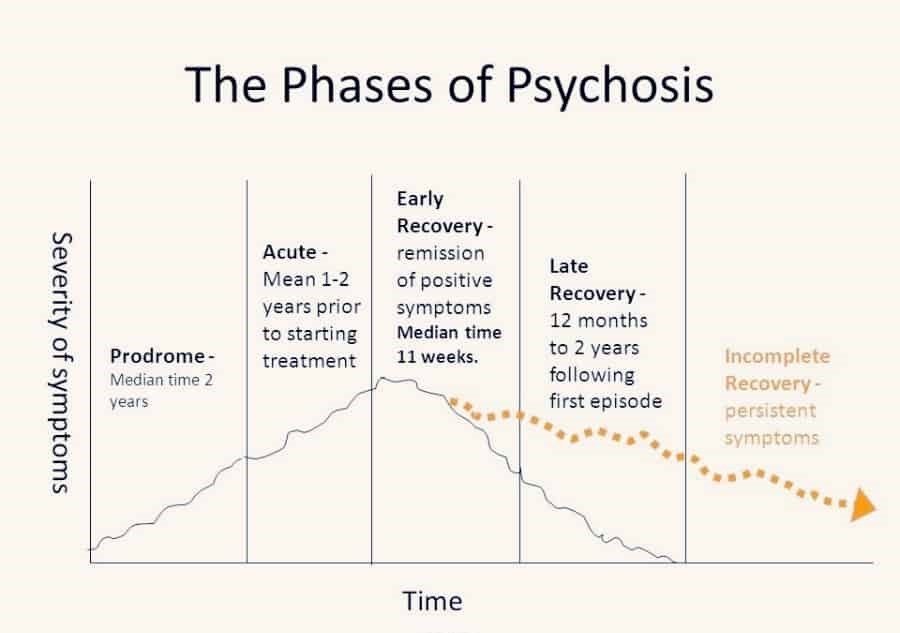
Digital Recreation and Its Influence on Psychosis
Immediately after understanding what psychosis entails, it becomes important to consider the broader aspects of lifestyle and recreational choices in managing this condition. Digital recreation, particularly through platforms like online casinos, has emerged as a significant area of interest in this context. For insights into this digital world, one can refer to the Best Online Casinos for Mental Wellness, a resource that delves into the dynamics of online gaming and its potential impact on mental health.
Studies have shown that controlled, responsible gaming can help improve concentration, decision-making skills, and provide a sense of achievement. It’s crucial, however, to approach this with caution, considering the potential risks of addiction, particularly for individuals with a history of mental health issues. Excessive gaming might lead to increased isolation, exacerbation of psychotic symptoms, or the development of unhealthy coping mechanisms. The key lies in moderation and the implementation of responsible gaming practices. It’s important for individuals with psychosis who engage in digital recreation to do so under guidance, with set boundaries to avoid the pitfalls of excessive gaming.
Types of Psychosis
As mentioned, psychosis may happen due to several health problems. A psychotic episode can be described by the underlying health condition. Below are different types of psychosis and underlying mental illnesses.
Bipolar Disorder
Psychosis is not a defining part of bipolar disorder. Many people have bipolar without experiencing any psychotic symptoms. However, sometimes bipolar patients on a manic high can experience psychosis. Depressive lows and extreme highs characterize bipolar. Researchers Hannah Ritchie and Max Roser state that bipolar disorder is estimated to affect around 1% of the population.
Schizophrenia
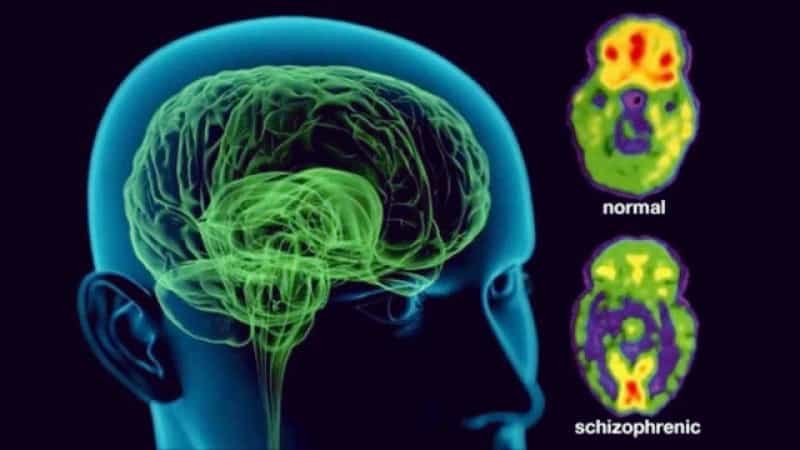
Schizophrenia is a lifelong condition. The first episode usually begins from around the age of 16 to 30. It is a severe condition, and patients can benefit from early intervention before the disease becomes acute. It is characterized by disordered thinking, hallucinations, and delusions. It requires lifelong treatment to manage symptoms.
Schizoaffective Disorder
Schizoaffective disorder has both symptoms of schizophrenia and bipolar disorder. In schizoaffective disorder, a person can have mood swings and mania, just like bipolar disorder. They may also have psychotic symptoms like schizophrenia for at least two weeks at a time.
Psychosis Caused by Drugs and Alcohol

Both drugs and alcohol can induce toxic psychosis. Stimulants that can have this effect include marijuana, cocaine, steroids, and amphetamines. Withdrawal from long term alcohol abuse can cause temporary delirium. Recovery involves addressing addiction.
Psychosis can also occur when a heavy user suddenly stops taking their drug of choice.
Delusional Disorder
Delusional disorder is associated with unshakeable beliefs in things that are not real. The condition was previously called paranoid disorder, and the person cannot be dissuaded that their belief is not real. The beliefs are not an entire fantasy but are often rooted in what could be possible. Examples include thinking a person is trying to poison them, or being deceived and conspired against.

Brief Mental Disorder
A brief mental disorder can happen when a person experiences extreme stress. The person may have been recently bereaved, for instance. The episode is usually short-lived, lasting a few days or weeks.
Organic Psychosis
Organic psychosis is the term applied to psychosis that is caused by an injury to the head or illness of the brain. Diseases of the brain, such as Huntington’s and Parkinson’s, can also cause organic psychosis.
Depressive Episode With Psychosis
For some people experiencing major depression, this can be accompanied by periods of psychosis.
Diagnosis of Psychosis Symptoms and Signals
In his article for the medical journal BMJ Open, Peter Byrne, consultant psychiatrist, writes that the symptoms of psychosis can be divided into positive and negative symptoms. Signs and signals to watch out for are detailed below.
Positive Symptoms of Psychosis
Delusions and hallucinations including:
- Unusual thoughts and feelings such as feeling they are being touched by something or someone.
- Believing that other people were spying on or following them
- Seeing something that is not there.
- Smelling things that others cannot smell
- Believing that a force or power is controlling them
Negative Symptoms of Psychosis
- A complete loss or a reduced ability to emotionally respond to people and the world around them
- A decrease in speaking
- Being withdrawn and unmotivated. The person may have difficulty in completing the simplest of tasks, such as getting dressed.
What Causes Psychosis?

Psychosis has a terrible stigma. Royals suffering from madness have long been hidden away as best as possible. But this approach lacks both compassion and empathy. There are various causes of psychosis that can affect just about anyone.
As mentioned above, those suffering from a psychiatric disorder suffer psychotic episodes. However, many people without a psychiatric disorder can have an episode of psychosis.
It’s estimated that around three percent of people will suffer from psychoses in their lifetime.
An otherwise healthy person can have psychosis during extreme periods of stress and anxiety. Lack of sleep, and travelling to foreign countries taking onboard new sensory experiences can also be causes of psychosis. The episode is usually temporary. In the elderly, age-related medical disorders can cause temporary psychotic episodes. An imbalance in potassium and sodium, as well as vitamin deficiencies and diabetes, can be causes of psychosis.
Postpartum or puerperal psychosis, while rare, is a severe illness that should be treated as a medical emergency. This type of psychosis is often overlooked as a case of the ‘baby blues.’ The baby blues are relatively common. Many mothers having carried a baby and given birth can experience a change in their hormones that causes a low mood.
Postpartum psychosis, however, occurs in around one to two in every thousand births. Delusions, mania, and hallucinations accompany a low mood. If any doubt at all, treat this kind of psychosis as a medical emergency. Call a doctor, a crisis team, or an ambulance for the sake of the baby’s welfare. Mothers are usually admitted to a mother and baby care unit. There they can receive treatment for their psychosis in a safe environment. It consists of medication and cognitive-behavioural therapy.
Diagnostics Used to Assess Psychotic Patients
Following an evaluation, a doctor may also order tests to eliminate or find out about any underlying conditions. Urine and blood tests can determine whether alcohol or drug abuse is the cause of symptoms. People can also have psychotic episodes when they are suffering from a brain tumour. The doctor may order CT or MRI scans to rule out this cause. A doctor may also ask a series of tests to determine the person’s level of cognition as well as personality tests.
Psychosis Treatment
If you suspect someone of being unwell, you must get the person treatment. But many people worry about how to help someone with psychosis.

We are all probably aware of someone who lives in our community who we consider ‘mad.’ The chances are they are just a little different and caught up in their reality. If a loved one or friend becomes unwell and is experiencing hallucinations and ‘fantastic‘ thoughts and beliefs, it’s no longer a joke.
For the majority of people, the reality of experiencing hallucinations is very frightening.
You must take a loved one you suspect of being unwell to a doctor who can refer them to a psychiatric team for assessment. A psychiatrist can assess their symptoms and the underlying causes of psychosis. It’s often the case that a person who needs treatment for psychosis is unwilling to get help.
The nature of psychosis is that the sufferer cannot comprehend reality fully and realize their need for help. In which case, you can contact a doctor on their behalf. You can get a doctor to visit, and they can refer your loved one to a psychiatrist for assessment and treatment.
Evaluation

The medical team will monitor the patient and observe their behaviour in a safe environment. They will also ask the patient a series of questions and evaluate their responses. Determining the cause of the psychosis is key to the treatment than prescribed. A person may have a drug or alcohol problem that has caused the psychosis. It may take in-patient care for some time to overcome the drug-induced psychosis. Or the psychosis may be short-lived, but the patient needs help to overcome a substance abuse addiction.
Medication
Psychosis usually responds well to medication. The doctor can prescribe the best antipsychotic medication to reduce and control the symptoms. Most people will take antipsychotic medications for a few days, weeks, or months. However, most schizophrenic patients need to take daily medications for the rest of their life. Similarly, bipolar patients who experience mania may also need to take drugs every day.

Cognitive-behavioural Therapy
Cognitive-behavioural therapy is an approach that is effective for patients. It involves meeting regularly with a mental health professional. Patients are encouraged to discuss how to change thought patterns and behaviours for the better. CBT can be used for patients who have symptoms that are not entirely treated with medication.
Support Groups

Support groups are extremely helpful for people who have experienced psychosis as reports the article published in the medical journal Schizophrenia Bulletin by the group of scientists (pp. 1211–1213). Psychosis is still a relatively rare issue and carries with it a stigma of sorts.
Trying to explain how you feel and felt to someone who has not had a psychotic episode can be intimidating. Support groups are proving to be an effective complementary support arm to other existing care. Self-expression and social support can help an otherwise isolated patient. Groups can help patients in meeting goals and sharing strategies and experiences.
Useful Resources and International Association

If you need support for dealing with a loved one with psychosis, then you can reach out to the team dealing with your loved one. You may be able to get time for a break if you have the role of a carer. Or you can join a peer-to-peer support group for a coffee and a chat.
Below is a list of useful resources and international associations.
ISPS
The ISPS promotes the social and psychological needs of people affected by psychosis.
International Bipolar Foundation
Find resources at the International Bipolar Foundation. There’s a suicide hotline, and bipolar patients can connect with others.
International Parkinson and Movement Disorder Society
Find resources about all aspects of Parkinson’s.
Mental Health America
This group helps Americans find local support groups. Many people find peer support helpful. Sharing stories and experiences can reduce feelings of loneliness and isolation.
The Balanced Mind Group
It is a group that has online communities. The group helps parents of children with mood disorders, bipolar disorder, and other related disorders.
Questions and Answers
Roughly 1.8% of Canadians and 10% of Americans are veterans. Many veterans go on to live meaningful and highly productive and successful lives with families and careers. However, the nature of combat can cause Post Traumatic Stress Disorder (PTSD). It’s estimated that up to 30% of combat veterans have PTSD in their lifetime.
That’s around 200,000 Canadian veterans and 6.12 million American veterans. Among combat veterans with PTSD, 30% to 40% report auditory or visual hallucinations and/or delusions, as stated in the book “Military Medicine” (pp. 273–277). The presence of psychotic symptoms in PTSD can be extreme and is similar to that of chronic schizophrenia.
The most distressing side effect for patients taking antipsychotic drugs is weight gain. And unfortunately, antipsychotics cause weight gain by stimulating the appetite. Patients feel hungry, take in more calories, and gain weight. Common antipsychotic drugs, olanzapine, and clozapine have a high risk of weight gain.
They bind strongly to the histamine H1 and serotonin 5-HT2C receptors causing the appetite to be stimulated. Jeannette Yeznach Wick’s book “Pharmacy Practice in an Aging Society” revealed that the average weight gain during the first year of treatment was 11.7 to 13.9 lb for clozapine and 15 to 26 lb for olanzapine. Obesity carries with it physical health problems. These include increased risk of stroke, cardiovascular problems, and diabetes.
In addition to physical health problems, people have a reduced quality of life when obese. It can lead to many patients to stop taking their medication and then suffering relapses in psychotic episodes. Patients are thirteen times more likely to stop taking medication due to drug-induced weight gain.
Strategies to avoid this involve switching drugs to those associated with a low risk of gaining weight. These include asenapine and haloperidol. Doctors can also prescribe weight loss drugs to take alongside antipsychotic medications. Also, discussing lifestyle changes can be beneficial in weight management.
As our overall healthcare improves, people are living longer. Unfortunately, with age comes a higher risk of dementia. According to the research of “The Alzheimer’s Research UK Dementia Statistics Hub” less than 2 percent of 65-69-year-olds suffer from dementia, but this increases to more than 20 percent for the 85-89-year-olds.
The nature and frequency of dementia symptoms vary throughout the illness, and psychotic features tend to present later on. Psychotic features include hallucinations, which are usually visual, delusions, and delusional misidentifications.
Their delusions may be out of context with their cultural and social background. Delusional misidentification, for example, might entail them suspecting that strangers are present. Or that family members are imposters. They may also not recognize their reflection. Alzheimer’s is estimated to have psychotic features in around 50% of patients. About 80% of dementia patients have psychotic hallucinations. Wandering while common in both dementia and Alzheimer’s is not a psychotic behaviour.
It can be a struggle knowing what to do if a loved one or even a stranger you see has psychosis. Mental hospitals are all too often portrayed in movies as asylums with authoritarian punishments. In Hollywood, patients are either restrained in straight jackets or drugged to pathetic non-existence of rocking to and fro.
Mental hospitals are not often frequented, and so the myths of how psychiatric patients are treated continue. If you meet a person who is living in an altered and false reality, then as a concerned citizen, what do you do? Could calling for help make their situation worse?
If you notice a change in a person’s behaviour. Or, if they are making risky decisions, then you should contact a treatment team. The person may have a card or details of a care or crisis team on their person. If not, you can call an ambulance. Psychiatric wards are not like draconian hell. They are safe places, and patients are not put in straight jackets to restrict their movements ever.
The only use for straight jackets these days maybe for prisoners. If the person is unsafe, agitated, and at risk of hurting themselves or others, the care team can administer rapid tranquilization. It is a fast-acting medicine that relaxes the patient almost immediately.
Not all people with psychosis respond immediately to treatment. As mentioned, three percent of people suffer from psychosis. So, it might be that you find yourself dealing with a family member that has ongoing psychosis. It can be upsetting, frustrating, and even annoying, listening to a loved one discussing ridiculous beliefs. But there’s a right and a wrong way to support the person. Here’s a DO and DON’T list to help you support a loved one with psychotic thoughts:
Criticize, correct, blame, confront, argue, or laugh. Don’t tell them they are psychotic but, at the same time, do not agree with their delusions. Don’t get angry and don’t take it personally.
Be calm, comforting, empathetic, share love, and a human connection. Ask about things they enjoy, focus on their strengths, ask about what is troubling them, and ask how you can help.
List of References
- Byrne P. (2007) Managing the acute psychotic episode, BMJ 2007: 334.
- Kingdon DG., Turkington D. (2005) Cognitive therapy of schizophrenia, Guilford Press, 219 p.
- Ritchie H., Roser M. (2018) Mental Health. Available at: https://ourworldindata.org/mental-health
- Castelein S., Bruggeman R., Davidson L., Gaag M. (2015) Creating a Supportive Environment: Peer Support Groups for Psychotic Disorders, Schizophr Bull. 2015 Nov; 41(6): 1211-3.
- Wick J. (2006) Pharmacy Practice in an Aging Society, CRC Press: Medical, 189 p.
- Nanji A.A. (1984) The psychiatric aspect of hypophosphatemia. Canadian Journal of Psychiatry 29: 599-600.
- Radua J., Borgwardt S., Crescini A., Mataix-Cols D., Meyer-Lindenberg A., McGuire PK., Fusar-Poli P. (2012) Multimodal meta-analysis of structural and functional brain changes in first episode psychosis and the effects of antipsychotic medication, Neurosci Biobehav Rev. 2012 Nov; 36(10): 2325-33.
- Murray E.D., Buttner N., Price B.H. (2012) Depression and Psychosis in Neurological Practice. In Bradley WG, Daroff RB, Fenichel GM, et al., editors: Neurology in clinical practice, ed. 6, Philadelphia, Butterworth-Heinemann, pp. 92-116.
- Bonnot O., Klünemann H.H., Sedel F., Tordjman S., Cohen D., Walterfang M. (2014) Diagnostic and treatment implications of psychosis secondary to treatable metabolic disorders in adults: a systematic review. Orphanet J Rare Dis. Apr 28; 9: 65.
